Breast Reconstruction
Pioneer of Direct-to-Implant Breast Reconstruction
Breast Reconstruction
Pioneer of Direct-to-Implant Breast Reconstruction
A breast cancer diagnosis is a traumatic event, and often it is the first time a woman needs serious medical care. After the shock, I hope you realize that breast cancer is a highly curable disease with highly effective treatments. That is why it is extremely important to not only seek out the right surgery for you, but to seek out the right surgeons, as how you look following mastectomy and reconstruction will profoundly affect you for what will be a long lived and normal life. For me, great mastectomy reconstruction really needs to look real, and suit the needs of the patient. Direct-to-implant breast reconstruction, also known as immediate breast reconstruction or one-stage reconstruction, is an advanced technique that allows women to wake up from their mastectomy surgery with natural-looking results, with no need for tissue expanders or additional surgeries.
Breast Reconstruction Topics on This Page
- Direct-to-Implant Breast Reconstruction
- Benefits Of Direct-to-Implant Breast Reconstruction
- Video: Advantages of One-Stage Breast Reconstruction
- One-Stage Breast Reconstruction—What to Expect
- How is One-Stage Breast Reconstruction Different?
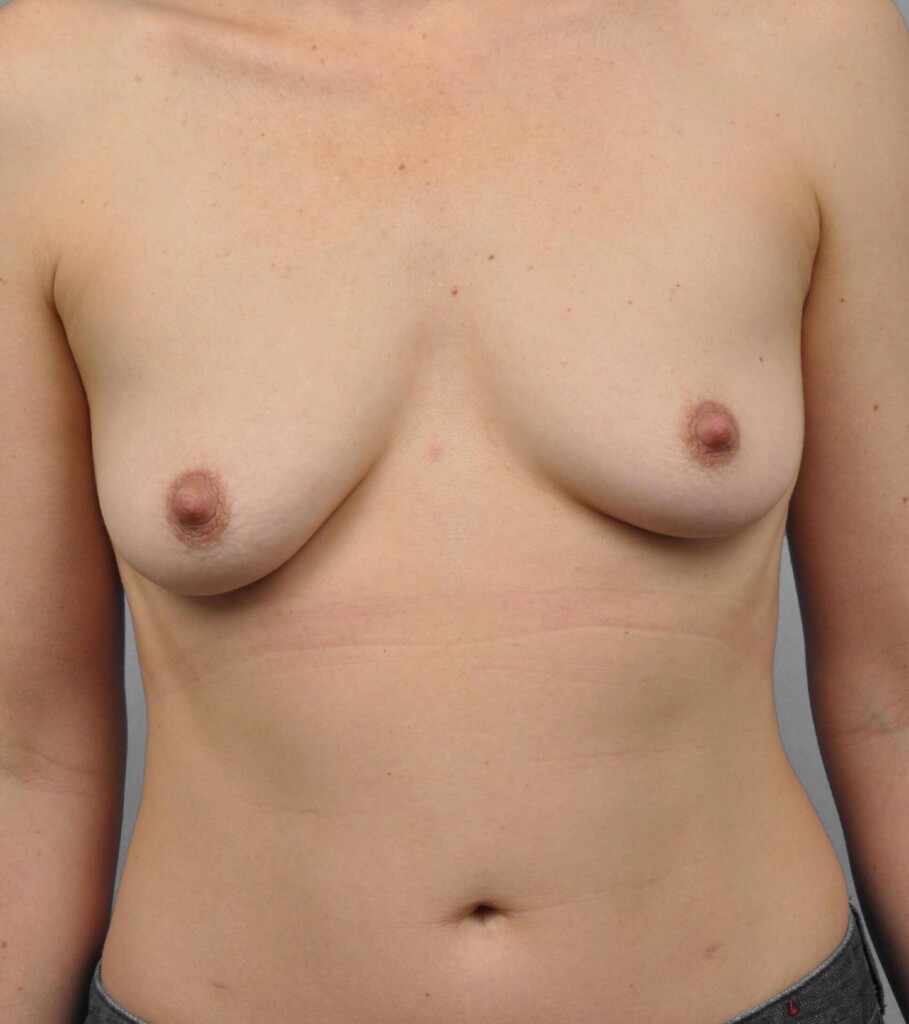
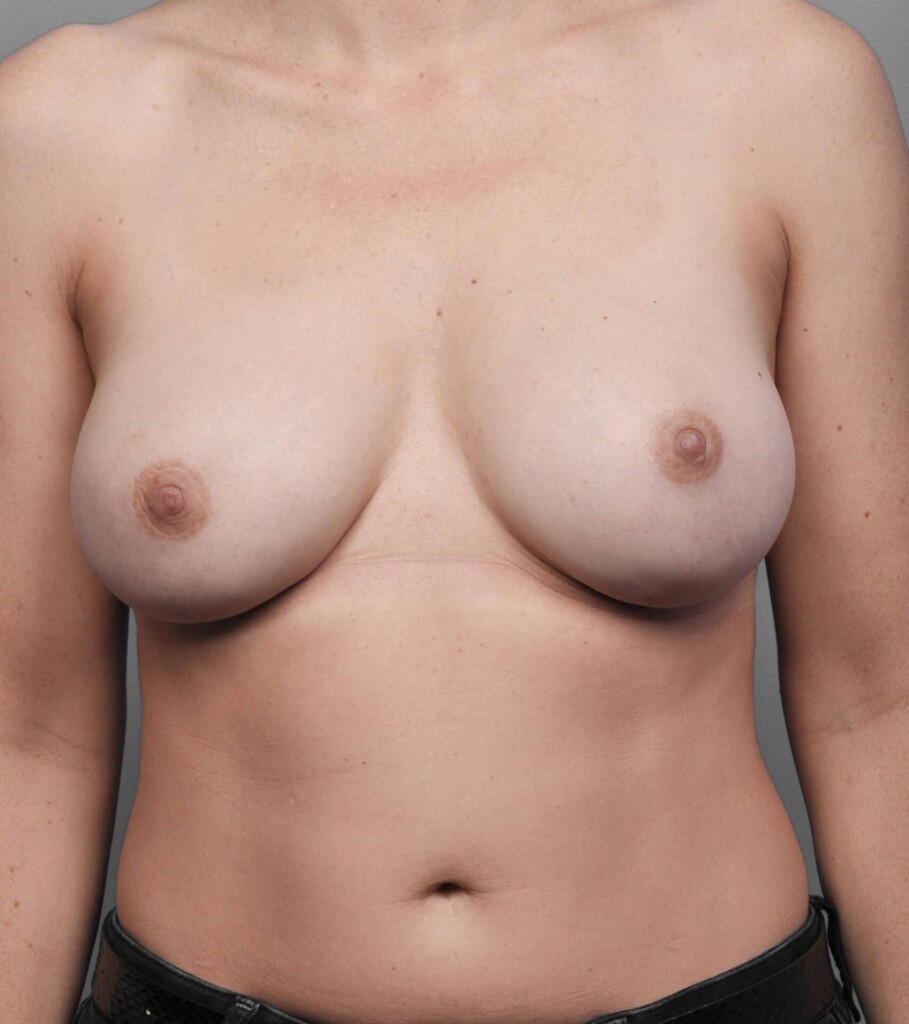
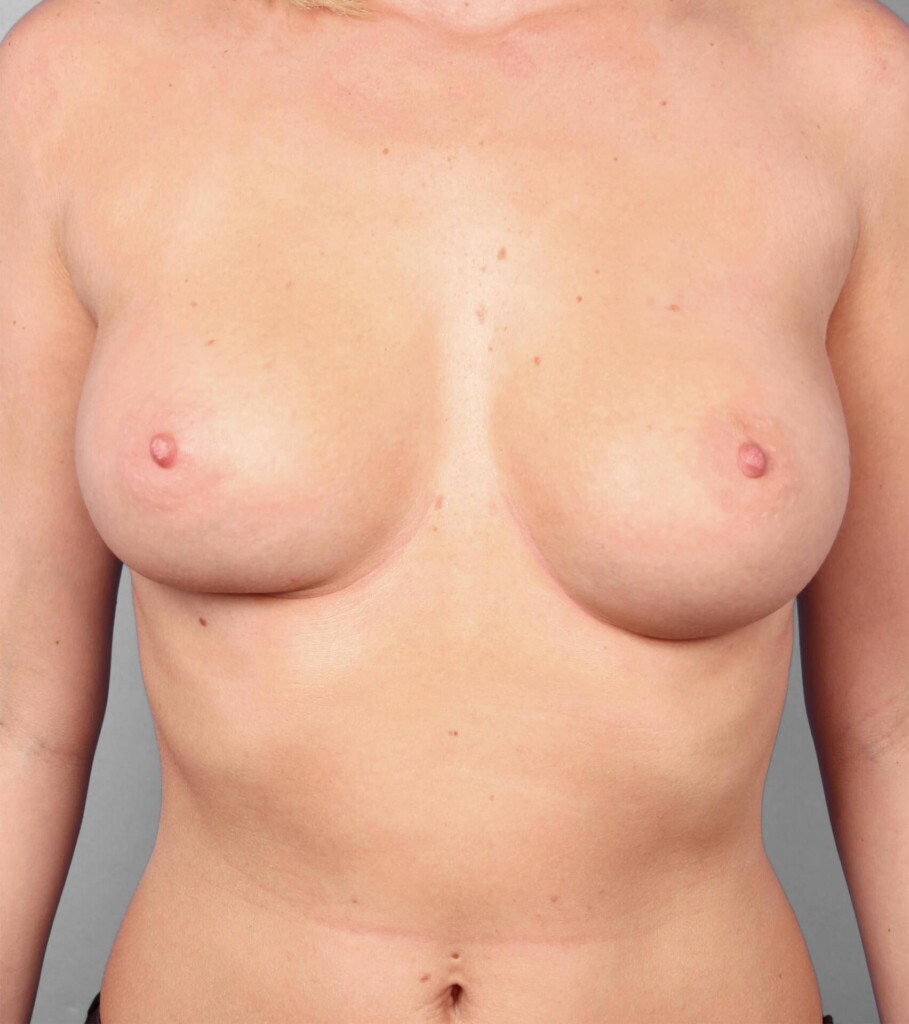
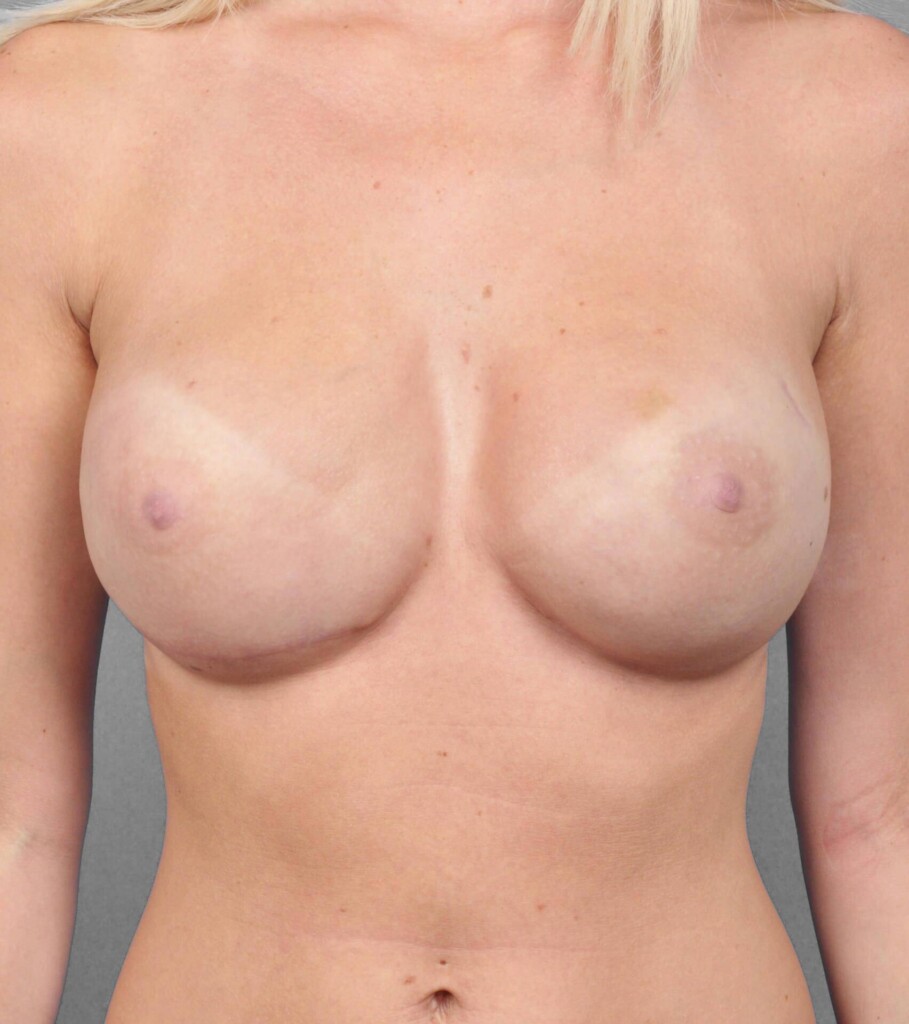
- Breast Reconstruction Before & After Photos
- Frequently Asked Questions
Direct-to-Implant Reconstruction in Los Angeles
Since 2005, it has been well accepted and safe to perform Nipple-Sparing mastectomies. This revolutionized breast reconstruction surgery, because the plastic surgeon no longer needed to stretch the skin with a tissue expander, since no skin was removed! As a young plastic surgeon, my patients pushed me to avoid the dreaded tissue expanders. What I found was that not only was a one-stage reconstruction possible, but it was also safer. I published my results in my original publication in 2012 in the Annals of Plastic Surgery.1
Over a decade later, the surgery continued to evolve. I no longer cut the pectoralis muscle, and place the implant over the muscle, supported by an internal bra made from acellular dermal matrix or absorbable mesh. This decreases pain, speeds recovery, and maintains strength. Nerve grafting can be combined with reconstruction, where the dominant sensory branches of the intercostal nerves can be connected to the sensory nerves on the dermis. This helps to improve sensation after surgery and diminishes pain and numbness.


DR. CASSILETH
BREAST SPECIALIST
Board-Certified Beverly Hills Plastic Surgeon, Breast Specialist, and Direct-to-Implant Breast Reconstruction Inventor
Benefits of One-Stage Breast Reconstruction
Women have come to me and expressed frustration with the traditional delayed reconstruction process. Some women who have already had reconstruction surgery are unhappy with their results. The truth is that the traditional plastic and reconstructive surgery process can be painful, requires multiple surgeries, and gives less-than-ideal outcomes. The traditional, standard goal of breast reconstruction has been to make you “look normal in clothes.” With Direct-to-Implant breast reconstruction, I uphold the new “standard of care” for breast reconstruction, which is “naked in the locker room” – you should feel comfortable and sexy with your new, reconstructed breasts, and confident that no one—even if you are changing in the locker room—will even be able to tell that you had breast cancer surgery.
Dr. Cassileth Discusses Advantages of One-Stage Breast Reconstruction
One-Stage Breast Reconstruction—What to Expect
Preparing for Direct-to-Implant Breast Reconstruction
The first step is a consultation appointment to discuss your medical history and your goals and perform an exam to determine if this type of procedure is right for you. We will review any specific pre-surgery instructions with you.
How Direct-to-Implant Breast Reconstruction Works
Every patient is unique and your surgical plan will depend on your individual anatomy and aesthetic goals. In general, reconstruction begins immediately after the oncological breast surgeon completes the mastectomy. I will create an internal bra using a dermal matrix to hold the implants in place, to create a beautiful and natural-looking result. Next, if we choose, I will connect deep nerves to the superficial nerves to help preserve breast sensation.
What to Expect After Mastectomy and Reconstruction
I go above and beyond to provide breast reconstruction patients with the highest level of post-surgical care. In surgery, we perform nerve blocks to minimize any post-surgical discomfort in the days after surgery. Our concierge nurse staff will provide detailed post-operative instructions and be available to help you heal and recuperate after your procedure. Learn more about post-surgery care by reading our recent blog ‘9 Tips for a Smooth Recovery‘.
How is One-Stage Breast Reconstruction Different?
I perform direct-to-implant, above-the-muscle reconstruction on almost every one of our mastectomy patients, with extremely low risk of complications and highly aesthetic results. So, why doesn’t everyone do this? Patients often hear they may not be good candidates for this technique from other doctors, or that expanders are “safer”. There are a few important choices that I have made that allow me to stand apart: the choice of the mastectomy surgeon; specific techniques designed to blend and support the implant; and a set of surgical and perioperative protocols that further increase the comfort and safety of the surgery.
1. Your Mastectomy Surgeon
In any mastectomy with reconstruction, two surgeons are involved: the breast surgeon (who does your mastectomy) and the plastic surgeon (who does your breast reconstruction after the mastectomy is complete). Obviously, having a great plastic surgeon is important to having a great result, but having an excellent mastectomy surgeon is equally critical. As a plastic surgeon, I can only give you the best aesthetic outcome when you have the best mastectomy surgeon. I exclusively work with breast surgeons who have demonstrated an extremely low risk of mastectomy flap necrosis, an unfortunately common complication that can cause death of the breast skin. My highly preferred surgeons are at BedfordBreastCenter.com, and have a mastectomy flap necrosis risk as low as 1%, when most surgeons have a rate of 30% or higher.
These breast cancer surgeons commonly employ nipple-sparing mastectomy and skin-sparing mastectomy techniques. They are highly experienced, and use only an incision at the crease under the breast—a feat that other surgeons find technically difficult, and that I insist on, because it improves your surgical outcome and the safety of the surgery.
2. Special implant Techniques
Next, I employ specific implant placement techniques to achieve natural-looking results. When it comes to the breast reconstruction portion of the procedure, the details make all the difference. First, the pectoral muscle is left intact, which means the recovery is far less painful, and avoids an unnatural-looking condition called “pec flex” deformity, where the pectoral muscle moves the breast upon flexing.
Second, I create an internal bra. Most plastic surgeons wrap the implant with acellular dermal matrix and place it under the mastectomy flap, which lets the implant droop to the bottom of the breast pocket and gives the implant very little support. I prefer installing a full internal bra prior to placing the implant, using an acellular dermal matrix or mesh to bridge the gap between the implant and the chest wall for a supported slope.This softens the contour of the implant, makes it look more natural, gives it room to shift slightly as a natural breast does, and decreases the need for fat grafting later.
Finally, I often reinnervate breast skin. During mastectomy surgery, the nerves which naturally pass through the breast tissue are removed, leaving the skin of the breast numb.2 Using an allogenic nerve graft, I reconnect the deep nerves to the superficial nerves, which allows for breast sensation. This is performed at the same time as the reconstruction, and the nerve regrows through the graft. Sensation improves as you heal.
3. Perioperative Details
Finally, I believe that key surgical and perioperative details further increase the comfort and safety of surgery. I use a Prevena VAC to seal the closure under a sterile, mild negative pressure dressing for five days after surgery. This lowers the risk of surgical infection and improves oxygenation of the wound edge, lowering complication rates. Next, I administer Exparel nerve-blocking injections during surgery, which blocks pain for three days after surgery. This comfort helps encourage early mobility after surgery (getting moving helps you recover faster!). I also inject PRF and peptides to the skin edge to encourage healing further and minimize visible scars. These substances, created by our own body, suppress inflammation and encourage revascularization and healing. This is further supported by postoperative hyperbaric treatments, which delivers oxygen to each and every healing cell in the surgical site and decreases surgical risks further. Our concierge nurse staff will follow you closely after surgery, which allows us to attend fully to your needs from day to day.
Frequently Asked Questions About Direct-to-Implant Breast Reconstruction and Sensation-Preserving Mastectomy
Surgical techniques have continued to improve, and experienced surgeons can now create a breast that often looks as good as, or better than the original. However, mastectomy typically leaves the breast and nipple numb. I am now happy to offer patients a nerve graft at the time of the mastectomy surgery and finally give patients an option to restore some sensation.
During the surgery, prior to the breast tissue removal, the large nerves exiting the chest wall are dissected before they enter the breast tissue. These are safely preserved so they are not removed with the mastectomy sensation. During the same surgery, and once the mastectomy is completed, these nerves are meticulously and carefully reconnected to severed nerve endings in the back of the skin, essentially providing a “jumper cable” around the breast implant. Patients typically start to notice sensation returning as early as three months after the mastectomy.
Sensation-preserving mastectomies are good options for women who want to preserve as much sensation as possible and are undergoing mastectomy. The nerves that are used are typically the lateral intercostal nerves, which enter the breast just behind the nipple and slightly to the side. The nerve that is used must be away from any area that may contain DCIS or breast cancer. Breast implant size may need to be limited depending on the individual patient’s anatomy.
Traditional mastectomy usually causes the loss of sensation to the some of the breast and nipple, more importantly light touch, which is protective, as well as pleasure sensation. That is because traditional mastectomy may cut the nerves that supply sensation to the majority of the breast skin and nipple. The cut nerves can even cause painful sensations or rarely, neuromas. With sensation-preserving mastectomy, a few months after surgery sensation will start to improve. The sensation will spread over the top of the breast until the area above the graft has reinnervated, which may take up to one year. Sensation is not normal, but is better than without the nerve graft.
Sensation-preserving mastectomy is best performed by a team of surgeons specializing in their unique skills, in which the mastectomy surgeon and the plastic surgeon work together to dissect the nerve at the beginning of the case and prior to the mastectomy, and that nerve remains undamaged during the mastectomy.
The operation is a microsurgical procedure and involves advanced training with nerve grafting. Following the reconstruction, the nerve is reconnected at the skin and chest wall using microsurgical techniques which involve advanced training. I am proud to be part of the first team to offer this operation in Southern California.
We often hear from patients that other surgeons have told them they “are not a candidate for direct-to-implant reconstruction.” They are told that it is too dangerous, and it only works for non-droopy, A- and B-sized breasts. Having performed hundreds of direct-to-implant reconstructions over more than 15 years, I can tell you that it’s not true. First, consider that it’s actually the first part of the surgery, the mastectomy, that is typically higher risk. For most breast cancer surgeons, the complication rate due to mastectomy flap necrosis is 30% or more.3 That means that most plastic surgeons are very wary of trying direct-to-implant reconstruction because they fear that the skin or nipple may die after the surgery. This would mean that the skin would need removal and closure. So they advise their patients to have a three-phase surgical process, with mastectomy and placement of tissue expanders, followed by three months of painful expansion, followed by surgery to replace the expanders with permanent implants. With our mastectomy surgeons, the risk of mastectomy flap necrosis is very low, around 1%. This means we can trust the breast skin, nipple, and areola to survive.
I believe tissue expanders are outdated and I hope that someday other centers can improve their techniques to make this a safe, commonly performed procedure. With a pre-pectoral implant that easily fits in place of the breast tissue, a tissue expander is not needed.
Direct-to-implant can be used in combination with other techniques where appropriate. For women with large or droopy breasts, I may use an “autoderm flap” which lifts and protects the implant and breast appearance at the same time; this is where extra skin is used to reinforce the implant position and a breast lift is done concomitantly to the mastectomy.
For patients who have undergone radiation therapy of the breasts, it is much safer to perform the reconstruction over the muscle, and also use the direct to implant techniques to minimize the increased risk of infection that comes with multiple implant surgeries. For patients with existing breast augmentation, the implants are usually placed under the muscle since the muscle is already partially detached from the chest wall.
Many women would like to avoid breast implants for reconstruction, and don’t want free flaps that take many hours and have extended recovery. There are a few options that allow implants and long surgeries to be avoided. First, of course, we can chose to “go flat”, which means that the breast is closed in a long line that has a smooth contour. This is also called “Aesthetic Flat Closure”. Here it is critical to avoid the dreaded “dog ear” or other unsightly skin bulges that ruin the result. Many, though, don’t want the long scar, and don’t want to be completely flat. For this group, we have the SWIM flap, a modification for smaller breasts that I am fondly calling the “K. Lo” after my patient who was too small for the SWIM techniques but avidly refused an implant. In these techniques, extra skin and subcutaneous fat is preserved and used to make a new, albeit much smaller, breast.
My SWIM breast reconstruction is an enhanced and refined version of the Goldilocks technique, but with preservation of the nipple and recruitment of any bra roll fat. Like direct-to-implant reconstruction, the SWIM breast reconstruction is carried out at the same time as a mastectomy, but involves creating a breast from the patient’s own existing tissue and fat instead of using an implant. My article, published in the Journal of the American College of Surgeons, details the procedure and proves the many benefits of this approach. The SWIM is ideal for larger-breasted women who want natural-looking, smaller breasts, as well as those who have undergone radiation treatments for cancer or who have multiple risk factors and health issues.
I perform more than 500 reconstruction cases each year. This includes Direct-to-Implant breast reconstruction, nipple reconstruction, reconstruction revisions, SWIM flaps, and fat grafting. Most of those cases are one-stage procedures—primary breast reconstructions done at the same time as the patient’s mastectomy—in our Beverly Hills surgery center.
I am dedicated to helping women live with confidence and comfort. During your consultation appointment, we will discuss your medical history and your aesthetic goals and I will answer any questions you have. If you are not an ideal candidate for single-stage reconstruction with saline or silicone implants, I will guide you to a procedure that is right for your needs and goals. -Dr. Lisa Cassileth
LET'S CHAT
Contact Us
We believe that the connection between the patient and the provider is at the heart of every successful procedure and look forward to meeting you in person to discuss your goals.

1 Cassileth L, Kohanzadeh S, Amersi F. One-stage immediate breast reconstruction with implants: a new option for immediate reconstruction. Ann Plast Surg. 2012 Aug;69(2):134-8. doi: 10.1097/SAP.0b013e3182250c60. PMID: 21734545.
2 Breastcancer.org Satisfaction with breast reconstruction results. Available: https://www.breastcancer.org/treatment/surgery/reconstruction/satisfaction Accessed April 19, 2024
3 Robertson SA, Jeevaratnam JA, Agrawal A, Cutress RI. Mastectomy skin flap necrosis: challenges and solutions. Breast Cancer (Dove Med Press). 2017;9:141-152. Published 2017 Mar 13. doi:10.2147/BCTT.S81712