Breast Implant Removal vs Replacement: Which Option Is Right for You?

Breast implants aren’t lifetime devices. At some point, most people with implants face the decision between breast implant removal or replacement. It’s a decision that deserves clarity, not pressure.
The right path depends on your health, anatomy, aesthetic goals, and the decade of life you’re in when the question arrives. There’s no universal answer, just the one that fits you.
Dr. Cassileth walks patients through explant surgery and replacement with the same care as a primary augmentation, so you decide based on your body, not online trends.
Key Takeaways
- Breast implant removal vs replacement is a personal decision shaped by your health, anatomy, lifestyle, and aesthetic goals.
- Explant surgery removes implants without placing new ones, while breast implant replacement exchanges old implants for new ones in the same operation.
- Capsular contracture, rupture, breast implant illness symptoms, and shifting preferences are the most common reasons patients pursue breast implant revision.
- Recovery from breast implant removal is generally shorter than recovery from implant removal and replacement, though both are outpatient procedures.
- A measurement-based consultation with a board-certified plastic surgeon produces the clearest path for your decision.
Why Do Breast Implants Need to Be Removed or Replaced?
Breast implants aren’t meant to last forever. According to the American Society of Plastic Surgeons, today’s implants typically last over a decade, with rupture risk rising about one percent every year they stay in place.
Most reasons patients pursue breast implant replacement fall into a few predictable categories:
- Capsular contracture or rupture.
- Rippling or shifting implants.
- Size dissatisfaction or evolving aesthetic goals.
- Breast implant illness symptoms include fatigue, joint pain, and cognitive fog.
- Lifestyle shifts from weight changes, pregnancy, or breastfeeding.
Health concerns also come up. A 2025 meta-analysis of 6,048 women found 81.9% experienced symptom improvement after explant surgery. Reviewing common breast implant illness myths before your consultation helps you distinguish between evidence and anecdote.
What Is Breast Implant Removal (Explant Surgery)?
Explant surgery removes one or both breast implants without placing new ones. Most patients come to the decision after months or even years of weighing whether to keep their implants at all.
During the procedure, your surgeon assesses the capsule, the scar tissue that naturally forms around every implant, and plans removal accordingly. Standard capsulectomy removes the implant with part or all of the capsule. En bloc capsulectomy removes both as a single intact unit.
A 2023 study in the Aesthetic Surgery Journal followed 150 patients for one year and found that 88% experienced at least partial symptom improvement, regardless of capsulectomy type. Some patients combine breast implant removal with a lift, while others let the tissue settle naturally into its post-explant shape.
What Is Breast Implant Replacement (Exchange Surgery)?
Breast implant replacement involves removing your current implants and placing new ones in the same operation. You may also hear it called implant exchange.
You can change size, switch from saline to silicone, choose a different profile, or upgrade to newer-generation options, such as Motiva implants that weren’t available during your original surgery.
Exchange also fixes problems. A 2025 revision surgery study of 133 patients found that over 80% reported high satisfaction after revision, whether they chose replacement or removal, making breast implant replacement a dependable path forward.
Breast Implant Removal vs Replacement: Key Differences
Seeing both options laid out side by side often helps the decision click.
The table below compares breast implant removal and replacement across procedure, anesthesia, time, recovery, final result, appearance, ideal candidacy, cost, and long-term maintenance, so you can weigh each factor against your own priorities.
| Factor | Breast Implant Removal (Explant Surgery) | Breast Implant Replacement (Exchange Surgery) |
| Procedure | Implants removed without replacement. Capsulectomy performed as en bloc, complete, or partial, depending on anatomy and indication | Implants removed and new implants placed in the same operation. Capsulectomy often performed to refresh the pocket |
| Anesthesia | General anesthesia, outpatient | General anesthesia, outpatient |
| Surgical time | Roughly 1 to 2 hours, longer if combined with a breast lift or en bloc capsulectomy on prior submuscular implants | Roughly 1.5 to 3 hours, longer if combined with a breast lift or pocket revision |
| Incision approach | Usually reuses the original incision along the inframammary fold or periareolar site | Usually reuses the original incision along the inframammary fold or periareolar site |
| Recovery timeline | Light activity within 1 to 2 weeks, full activity around 4 weeks | Light activity within 1 to 2 weeks, full activity closer to 4 to 6 weeks, similar to primary augmentation |
| Final result timeline | Tissue settling and “fluffing” over 3 to 12 months | Implant settling (“drop and fluff”) over 3 to 6 months |
| Breast appearance | Smaller, more natural breast contour reflecting native tissue after fluffing | Retained or refined breast volume with a new size, shape, profile, or implant type |
| Ability to change size, type, or profile | Not applicable, no new implant placed | Full opportunity to adjust size, switch saline to silicone, refine profile, or upgrade technology |
| Addresses capsular contracture | Yes, when combined with capsulectomy | Yes, when combined with capsulectomy and often a plane change |
| Addresses rupture | Yes, removes ruptured implant and capsule | Yes, removes ruptured implant and replaces with a new, intact device |
| Addresses implant illness concerns | Yes, a common reason women choose this route | Possible, though many patients exploring systemic symptoms choose removal alone |
| Ideal candidate | Patients who no longer want implants, have persistent health concerns, or prefer simplified future screening | Patients who want to maintain breast volume while refreshing size, shape, or addressing a complication |
| Long-term maintenance | No further implant monitoring needed | MRI or ultrasound screening beginning 5 to 6 years after surgery, continuing every 2 to 3 years per FDA guidance |
| Typical cost | Generally lower than replacement, though added lift or complex capsulectomy increases price | Generally higher, reflecting new implant cost plus potential pocket revision |
| Insurance coverage | Sometimes covered when medically indicated (rupture, contracture, reconstruction) | Rarely covered unless tied to reconstruction or documented complication |
The right choice comes down to your goals, anatomy, and priorities. The table gives you a useful overview, but a consultation is where those variables turn into a plan built around you.
When Is Breast Implant Removal the Right Choice?
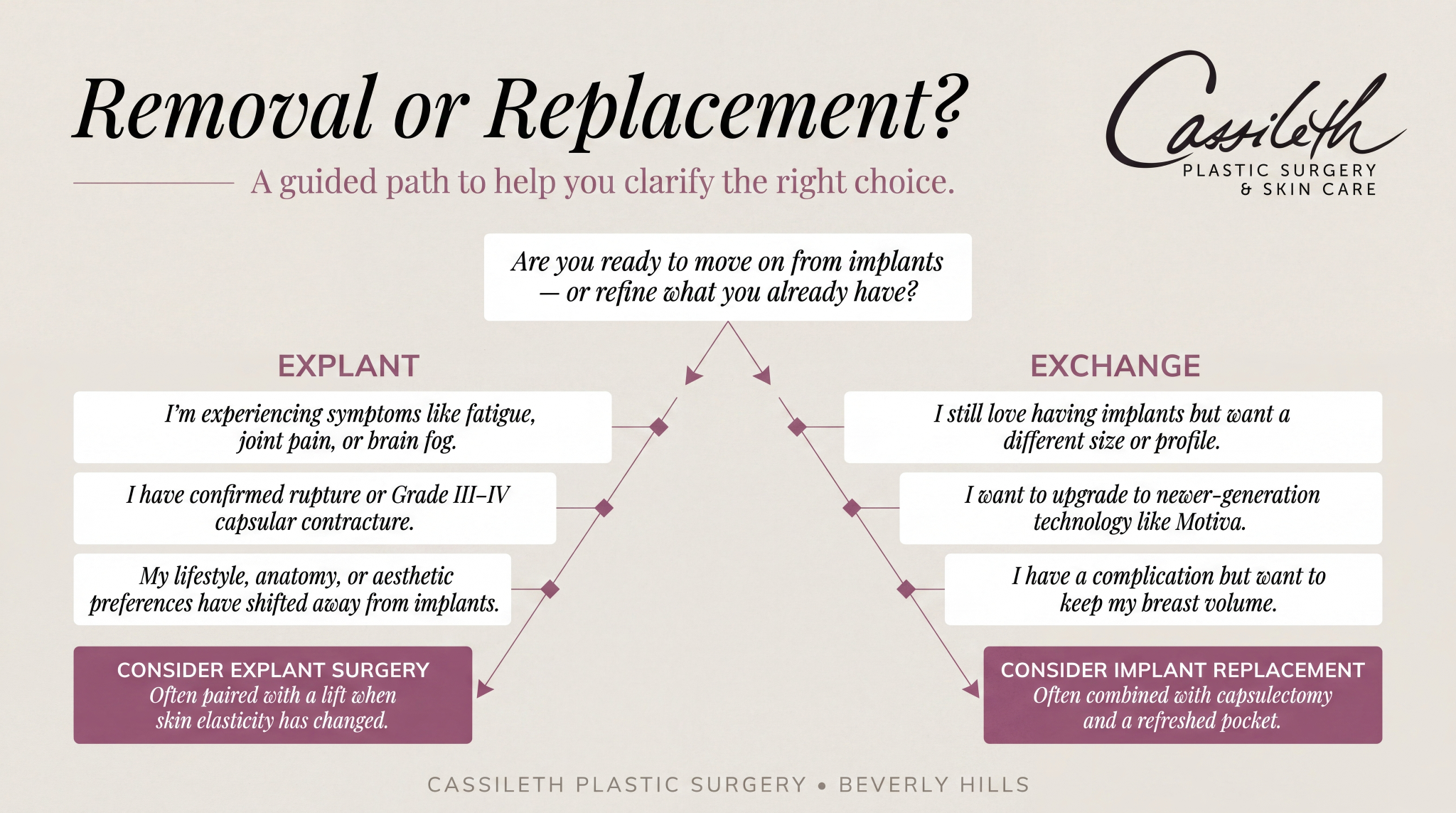
For some patients, explant surgery alone is simply the better path. The reasons usually fall into two groups: health-driven and lifestyle-driven.
Health and Medical Reasons
Health often drives the decision to pursue breast implant removal.
Capsular contracture that has progressed to Baker Grade III or IV, with visible firmness or distortion, usually warrants removal, especially if you don’t want a new implant.
A confirmed rupture also triggers it. That’s why the American Society of Plastic Surgeons echoes FDA guidance recommending MRI or ultrasound screening five to six years after silicone placement, then every two to three years, since ruptures are often silent and easy to miss without imaging.
Suspected breast implant illness symptoms, like fatigue, joint pain, or brain fog, also push many patients toward breast implant revision without replacement.
Lifestyle and Personal Reasons
Not every removal is driven by a clinical event. Sometimes, your implants simply stop aligning with your body image or lifestyle. Common reasons patients choose removal include:
- Endurance athletics or an active lifestyle implants now interfere with.
- Post-pregnancy or post-weight-loss body shifts.
- Evolving aesthetic taste that favors a more natural look.
- A desire to simplify future health screenings, since mammograms can get more complex with implants in place.
Breast implant revision that ends with removal is a valid path whenever your priorities have shifted.
When Is Breast Implant Replacement the Right Choice?
Updating Size, Type, or Profile
If you still love having implants and want to refine the look, breast implant replacement is usually the more satisfying path. Many patients upsize modestly, downsize for better proportion after pregnancy, or switch from saline to silicone for a softer feel.
Upgrading to newer-generation technology at the same time gives you a decade’s worth of implant engineering, with refined shell cohesiveness, better projection options, and improved rippling resistance.
Addressing Complications While Maintaining Volume
Replacement is often the better path when a complication develops, but you still want your breast volume.
Capsular contracture, for instance, can be corrected with a capsulectomy and a new implant, often paired with a plane change from subglandular to submuscular for better long-term coverage.
Malposition, bottoming out, asymmetry, and confirmed rupture all respond well to carefully planned exchange surgery. Implant removal and replacement with internal capsule adjustment is one of the most common forms of breast implant revision that Dr. Cassileth performs for returning patients.
What Happens to Your Breasts After Implant Removal?

After explant surgery, your appearance depends on several factors:
- Your original implant size.
- Skin elasticity and age.
- Pregnancy and breastfeeding history.
- How long your implants were in place.
Smaller implants paired with strong elasticity often look natural within weeks, while larger or long-standing ones can leave tissue looser early on. Then comes the “fluffing” process, where your natural tissue rebounds into the empty pocket over three to twelve months.
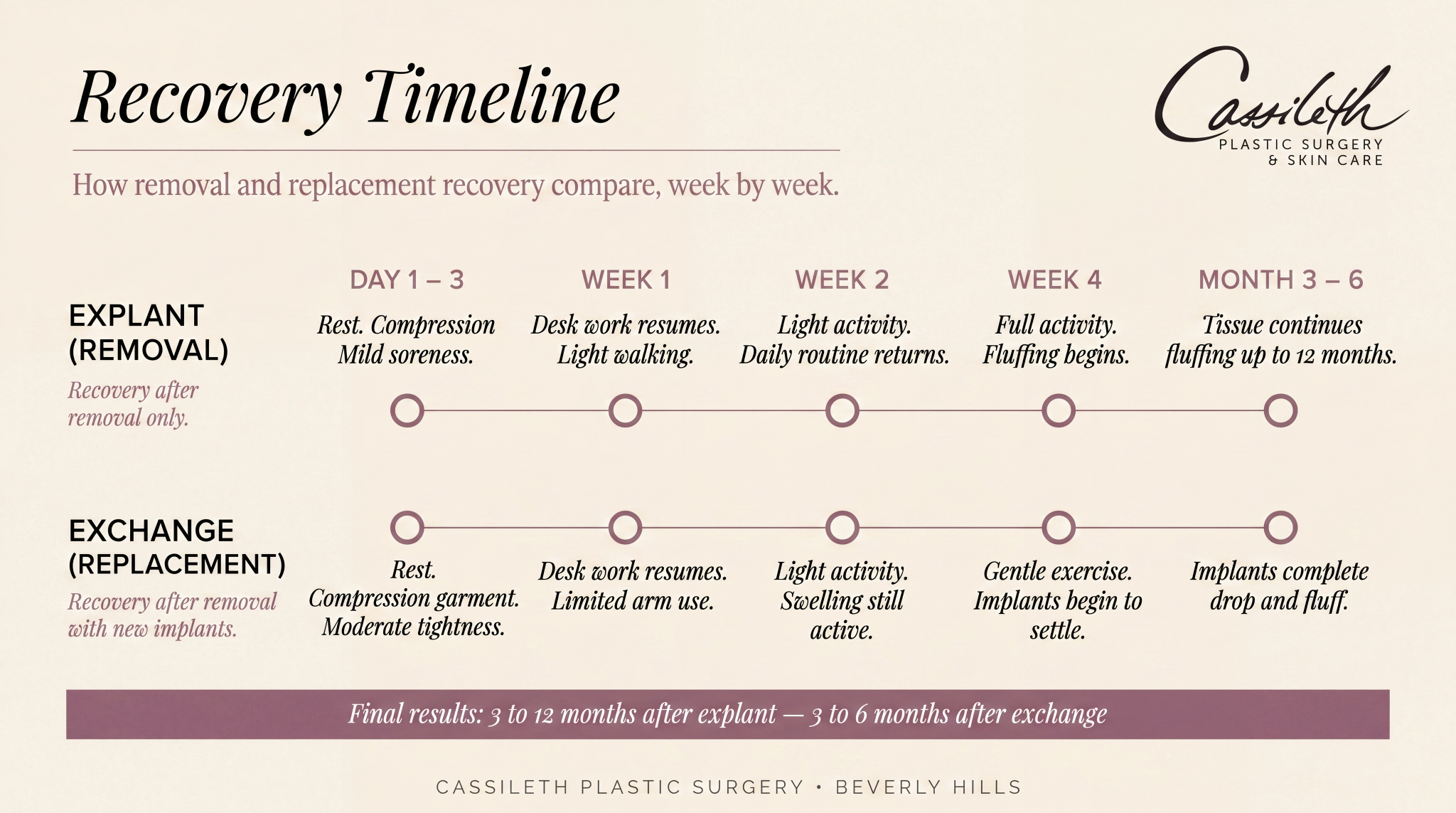
Recovery: Removal vs Replacement
Recovery timelines differ between the two procedures. According to the Cleveland Clinic, patients typically avoid strenuous activity for one to two weeks, with tenderness lasting up to six weeks, and final results becoming fully apparent three to six months after either procedure.
| Factor | Explant Surgery (Removal only) | Breast Implant Replacement |
| Light activity | Within 1 to 2 weeks | Within 1 to 2 weeks |
| Desk-based work | Around 1 week | 1 to 2 weeks |
| Full activity / vigorous exercise | Around 4 weeks | 4 to 6 weeks |
| Final settling | 3 to 12 months (tissue fluffing) | 3 to 6 months (drop and fluff) |
| Typical discomfort | Modest, often lighter than expected | Closer to original augmentation recovery |
| Factors that extend recovery | Capsulectomy, added breast lift, healing profile | Capsulectomy, pocket revision, added lift, healing profile |
Questions to Discuss with Your Surgeon (How to Decide?)
A few honest questions can clear up whether breast implant removal or replacement is the better path for you:
- Do you want to maintain your breast volume, reduce it, or return to your natural chest?
- Are you experiencing symptoms you think may be linked to your implants?
- How do you feel about the ongoing maintenance implants require?
- What are your long-term aesthetic goals, not just today’s?
- Does your current lifestyle still align with carrying implants for another decade?
Your answers give Dr. Cassileth the clarity to tailor a plan around you. The consultation is where that clarity actually happens, and a rushed decision rarely produces the result you want. There is no extra credit for choosing quickly, so Dr. Cassileth gives the process the time it truly deserves.
Choosing the Right Surgeon For Your Treatment

Breast revision and explant surgery demand more skill than a primary augmentation. Your surgeon has to navigate capsule quality, scar tissue planes, and previous pocket boundaries to deliver a balanced result.
That’s why board certification and breast specialization matter.
Dr. Cassileth routinely performs breast implant revision, with a widely recognized 95% cure rate for capsular contracture, and treats each case as a tailored decision rather than a templated one.
So, Removal or Replacement? What’s Next for You?
Neither breast implant removal nor replacement is universally better. The right choice depends on your health, comfort, and long-term goals. Some women choose explant surgery to end their relationship with implants, while others prefer breast implant replacement to refine size, profile, or address a complication.
A consultation is where clarity happens. Schedule a consultation with Dr. Cassileth in Beverly Hills to walk through your history, measurements, and goals, and decide with confidence.
FAQs
How do I know if I should remove or replace my breast implants?
The decision between breast implant removal vs replacement is usually clarified during a consultation covering your history, symptoms, anatomy, and goals. If you still want volume, replacement fits. If you’re ready to move on, explant surgery often works better.
What does breast implant removal look like without replacement?
Appearance after breast implant removal depends on your skin elasticity, original implant size, and how long the implants were in place. Many women experience initial deflation, then a three-to-twelve-month fluffing period as tissue rebounds into the empty pocket.
Can I get a breast lift at the same time as implant removal?
Yes, a breast lift pairs naturally with explant surgery when skin elasticity is reduced. Combining them delivers a lifted, contoured silhouette in one procedure, which many patients choosing breast implant removal or replacement without added volume find essential.
How often should breast implants be replaced?
Implants aren’t lifetime devices. Most women revisit the decision between ten and twenty years after surgery. FDA guidance recommends MRI or ultrasound screening 5 to 6 years after placement, then every 2 to 3 years, prompting breast implant revision when needed.
Is explant surgery covered by insurance?
Insurance sometimes covers explant surgery when medically indicated, including confirmed rupture, severe capsular contracture, infection, or reconstruction. Breast implant removal for purely cosmetic reasons is generally not covered. Coverage varies, so clarify documentation and pre-authorization during your consultation.

Lets Chat!
Contact Us
We believe that the connection between the patient and the provider is at the heart of every successful procedure and look forward to meeting you in person to discuss your goals.
